ABSTRACT
BACKGROUND: Keloid tissues contain inflammatory cells and upregulated pro-inflammatory cytokines.1, 2 The Janus kinase (JAK)-signal transducer and activator of transcription (STAT) pathway mediates cellular responses to these cytokines (Figure 1). These cellular responses include proliferation, differentiation, migration, apoptosis, and cell survival, depending on the signal, tissue, and cellular context3; hence influencing the process of inflammation and fibrosis.4 JAK-inhibitors belong to a new class of therapeutics that interferes with the JAK-STAT pathway. These drugs are currently used for different indications, ranging from myeloproliferative disorders such as myelofibrosis and polycythemia vera, to inflammatory disorders such as rheumatoid arthritis and atopic dermatitis.5 It has been reported that JAK-inhibitors may also have a role in the treatment of keloids, by targeting inflammatory and proliferative processes in keloid formation and progression.6, 7 To aim of the study is to critically review the role of the JAK-STAT pathway in keloid pathogenesis and the evidence for JAK-STAT inhibitors in keloid treatment in current literature.
MATERIALS AND METHODS: The search combined the terms (1) keloid and (2) JAK and/or TYK and/or STAT and included MeSH terms and synonyms. Two reviewers screened the articles and assessed the full-texts on eligibility. Data were collected on the tested drugs and molecules, the type of cells and tissues used in the experiments, and study findings on the association between the JAK-STAT pathway and keloid cells and tissues.
RESULTS: From a total of sixteen included preclinical studies, twelve different JAK and/or STAT inhibitors were investigated. All tested drugs inhibited keloid progression as demonstrated by different processes, including reduced collagen production, cell proliferation and migration, increased cell cycle arrest and apoptosis, decreased (paracrine) signalling, and decreased profibrotic gene expression. Five studies reported elevated JAK and/or STAT expression in keloid cells and tissues without involving drug testing. No clinical studies have been performed to date.
CONCLUSION: Preclinical studies indicate a role for the JAK-STAT pathway in keloid pathogenesis and JAK-STAT inhibitors in keloid treatment. The effect of these drugs should be further investigated on relevant biomarkers in a human keloid skin model, preferably including immune cells besides keloid fibroblasts and keratinocytes. Moreover, a study with keloid patients is necessary to acquire clinical data.
REFERENCES:
1. Ogawa R. Keloid and Hypertrophic Scars Are the Result of Chronic Inflammation in the Reticular Dermis. Int J Mol Sci. Mar 10 2017;18(3)doi:10.3390/ijms18030606
2. Dong X, Mao S, Wen H. Upregulation of proinflammatory genes in skin lesions may be the cause of keloid formation (Review). Biomed Rep. Nov 2013;1(6):833-836. doi:10.3892/br.2013.169
3. Harrison DA. The Jak/STAT pathway. Cold Spring Harb Perspect Biol. Mar 1 2012;4(3)doi:10.1101/cshperspect.a011205
4. Bharadwaj U, Kasembeli MM, Robinson P, Tweardy DJ. Targeting Janus Kinases and Signal Transducer and Activator of Transcription 3 to Treat Inflammation, Fibrosis, and Cancer: Rationale, Progress, and Caution. Pharmacol Rev. Apr 2020;72(2):486-526. doi:10.1124/pr.119.018440
5. Welsch K, Holstein J, Laurence A, Ghoreschi K. Targeting JAK/STAT signalling in inflammatory skin diseases with small molecule inhibitors. Eur J Immunol. Jul 2017;47(7):1096-1107. doi:10.1002/eji.201646680
6. Lim CP, Phan TT, Lim IJ, Cao X. Stat3 contributes to keloid pathogenesis via promoting collagen production, cell proliferation and migration. Oncogene. Aug 31 2006;25(39):5416-25. doi:10.1038/sj.onc.1209531
7. Zhou Y, Sun Y, Hou W, et al. The JAK2/STAT3 pathway inhibitor, AG490, suppresses the abnormal behavior of keloid fibroblasts in vitro. Int J Mol Med. Jul 2020;46(1):191-200. doi:10.3892/ijmm.2020.4592
©
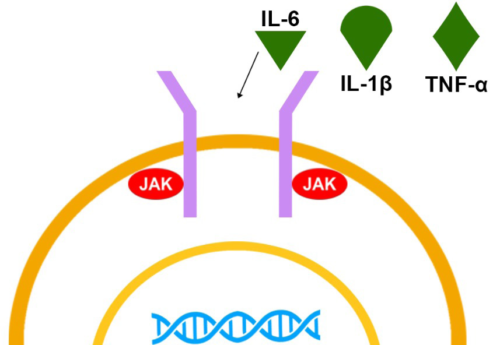
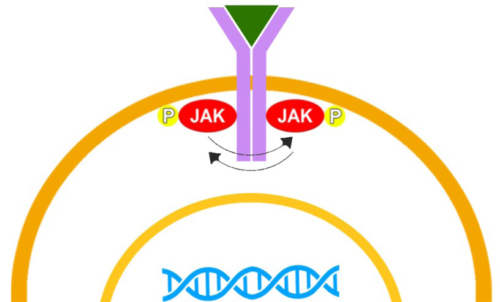
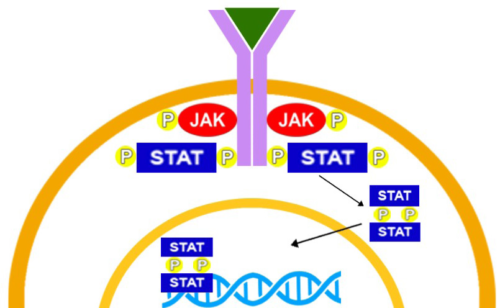
Figure 1. Activation of the JAK-STAT pathway
a: The cell membrane contains JAK-STAT components. The extracellular site of these JAK-STAT components functions as a receptor for ligands, such as cytokines and growth factors. The intracellular site is associated with JAK proteins.
b: The JAK-STAT components dimerize after ligand binding. The JAK proteins then phosphorylate each other.
c: Trans-phosphorylated JAKs then phosphorylate the receptors, creating docking sites for STAT proteins. STAT proteins dock to these specific domains, are then phosphorylized by JAKs, dissociate from the receptor and dimerize. This dimer then translocates to the cell nucleus and attaches to the DNA for transcription, eventually resulting in gene expression.
